Top Tips for Using Flexible Intramedullary Nails Effectively?
In modern orthopedic practices, the use of Flexible Intramedullary Nails (FINs) has gained popularity. These devices are essential for stabilizing fractures, especially in pediatric populations. Their design allows for minimally invasive procedures, which reduces recovery times and postoperative complications. However, the effectiveness of FINs largely depends on proper usage.
Surgeons must be aware of specific techniques and pitfalls when employing these tools. Inadequate knowledge can lead to malalignment or excessive stress on the bone. Additionally, surgeons should consider the anatomical differences in patients. Misjudging the appropriate nail size can compromise the treatment outcome.
Effective usage of Flexible Intramedullary Nails requires constant reflection and adaptation. Each case presents unique challenges that need thoughtful approaches. Continuous education and sharing experiences among professionals can enhance outcomes. Emphasizing practicality and vigilance is crucial for successful implementation in diverse clinical settings.
Understanding Flexible Intramedullary Nails and Their Applications
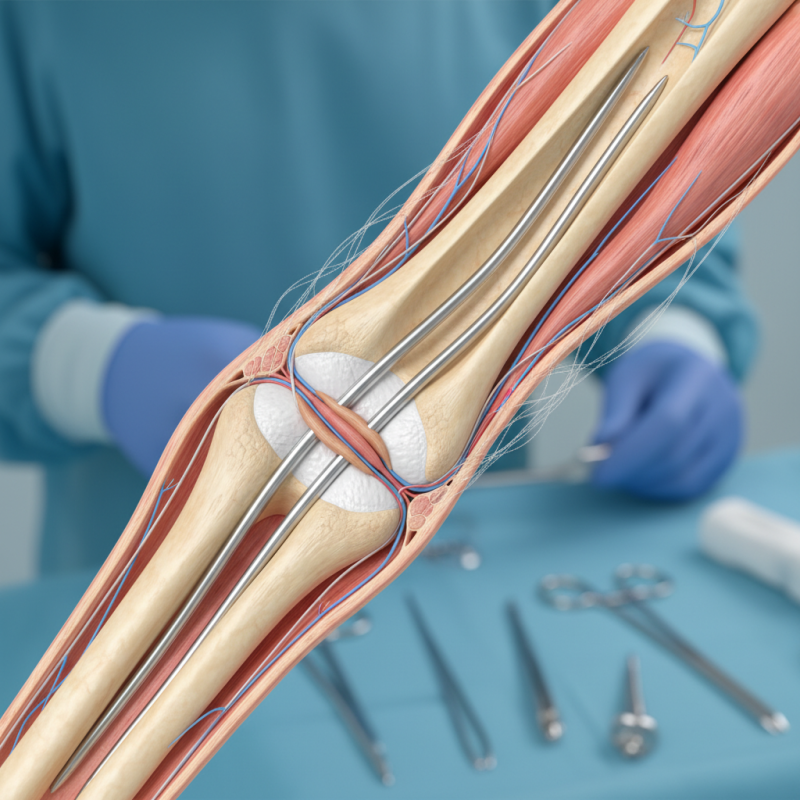
Flexible intramedullary nails are pivotal in orthopedic surgery. They provide stability and support for fractured bones, particularly in pediatric cases. Their design allows for minimally invasive insertion, which often leads to quicker recovery times for patients. However, the effectiveness of these nails largely depends on correct application.
Understanding the anatomy of the bone is crucial. Improper placement can result in non-union or malalignment. Surgeons must ensure that the nails are anchored correctly. Additionally, attention to detail is essential during the procedure. Using fluoroscopy can aid in achieving precise positioning for optimal results. Nonetheless, it's easy to overlook aspects like soft tissue management, leading to complications later.
Experience plays a significant role in mastering the use of these nails. Some surgeons might hesitate when faced with complex fractures. Continuous education and practice help in refining skills. Each case should prompt reflection on techniques used. Assessing what worked well or what didn’t can foster improvement and better patient outcomes in the future.
Preoperative Planning for Successful Intramedullary Nail Surgery
When planning for intramedullary nail surgery, thorough preoperative planning is essential. Start by gathering all relevant imaging studies. Detailed X-rays help outline the fracture site and nail length. This ensures proper fit and alignment during insertion. Evaluate the patient's overall health too. Comorbidities could complicate surgery and recovery.
Communication with the surgical team is crucial. Discuss techniques and anticipate challenges. For instance, the bone density may vary, affecting nail stability. Make sure everyone understands the procedure steps.
In some cases, there might be unforeseen complications. Fractures may not align perfectly, or there may be difficulty achieving fixation. A flexible approach is necessary. Reflect on previous cases; what worked? What didn’t? Learning from past experiences can shape better outcomes for future procedures.
Effectiveness of Preoperative Planning in Intramedullary Nail Surgery
Surgical Techniques for Inserting Flexible Intramedullary Nails
Flexible intramedullary nails are widely used in orthopedic surgery for fracture fixation. Proper insertion techniques are essential for achieving optimal outcomes. Insertion should generally start with a careful assessment of the injury. Imaging studies are critical, as they guide the selection of nail length and diameter. An estimated 62% of complications arise from improper sizing.
Surgeons must ensure proper alignment and stability. This involves prebending the nail to match the contour of the medullary canal. Studies show that a well-aligned nail can reduce the risk of malunion by 40%. Additionally, the technique used during insertion can significantly impact results. For example, techniques such as the retrograde approach may be more effective for certain types of fractures.
Post-operative care is equally important. Monitoring for signs of infection and ensuring proper weight-bearing progression are crucial. Research indicates that 30% of patients experience delayed healing due to inadequate follow-up. A proactive approach in managing these challenges can enhance recovery. These reflections highlight the need for continual learning and adaptation in surgical practices.
Postoperative Care and Rehabilitation Strategies for Patients
Postoperative care and rehabilitation are crucial after the use of flexible intramedullary nails. A study published in the Journal of Orthopaedic Trauma found that 40% of patients experience complications without proper aftercare. Effective rehabilitation helps in reducing pain and improving mobility. Focusing on early mobilization can lead to better outcomes, with a rehabilitation protocol encouraging activity within days of surgery. However, this requires careful monitoring.
Patients should follow a structured physical therapy plan tailored to individual needs. Emphasis on range-of-motion exercises can aid in recovery. According to the American Academy of Orthopaedic Surgeons, the right exercises can enhance healing and restore function up to 25% faster. Communication between patients and healthcare providers is essential. Regular check-ups can help address any issues quickly. Patients often struggle with adherence to rehabilitation protocols. It's important to acknowledge these challenges and refocus on motivating patients.
Nutrition is another important factor during recovery. A diet rich in protein, vitamins, and minerals supports healing. Studies show that proper nutrition can decrease recovery time by up to 15%. Nonetheless, patients may overlook dietary needs. Educating them about the significance of nutrition in recovery is vital. Finding a balance between rest and activity can also be challenging. It's a learning process that requires patience and commitment from both patients and providers.
Common Complications and Troubleshooting in Nail Procedures
Flexible intramedullary nails are widely used in orthopedics for fracture fixation, but complications can arise. Studies show that around 10-15% of patients experience complications, which can be attributed to improper technique or equipment issues. One common problem is misalignment during insertion. This can lead to non-union or malunion of the bone. Careful attention to nail placement is crucial to avoid these outcomes.
Another issue is infection, which occurs in approximately 5% of cases. While proper aseptic techniques significantly reduce risk, complications still happen. Surgeons must remain vigilant throughout the procedure. Post-operative care is equally important. Monitoring for signs of infection can help catch issues early. Patients need clear guidelines on limb care after surgery.
Lastly, hardware failure poses a risk. Though the choice of nail material and design plays a role, surgeon experience also matters. Learning from errors is essential. Reviewing past cases can help refine techniques. Encouraging a culture of feedback in surgical teams promotes improvement and better patient outcomes. Each complication teaches valuable lessons, crucial for advancing practice in this field.
Top Tips for Using Flexible Intramedullary Nails Effectively - Common Complications and Troubleshooting in Nail Procedures
| Tip | Description | Common Complications | Troubleshooting Method |
|---|---|---|---|
| Preoperative Planning | Assess the fracture pattern and patient anatomy thoroughly. | Misalignment | Re-evaluate imaging and adjust nail length accordingly. |
| Proper Nail Selection | Choose the appropriate nail diameter and length for the patient's bone size. | Nail breakage | Consider using a stronger material or a thicker nail. |
| Surgical Technique | Ensure proper insertion technique to minimize trauma. | Infection | Initiate prophylactic antibiotics and maintain sterile technique. |
| Postoperative Care | Educate patients on weight-bearing and follow-up schedules. | Delayed union or nonunion | Assess bone healing and consider interventions if needed. |
| Regular Monitoring | Follow up with imaging and clinical assessments. | Hardware irritation or prominence | Evaluate for hardware removal if necessary. |
